Adolescence – that interesting, exciting, and challenging period of life that ever one of us has to go through. Of course, some seem to stay perpetually stuck there emotionally, long after they’ve left their teen years behind. But for most, it’s a several-years-long transition from childhood to adulthood. The journey is often bumpy, even for the teens that seem to have things reasonably together.
 Unfortunately, though, some teens really struggle during this phase of life – beyond what would (or should) be considered normal adolescent ups and downs. It can be hard, as a parent, to know when to take the attitude of “this, too, shall pass” versus “it’s time to seek professional help for our son / daughter”. Sometimes there’s a significant gray area, and multiple factors need to be considered. But more often than not, the signs are pretty clear – if you’re paying attention; that can be a challenge for parents with harried schedules and plates overflowing with obligations and responsibilities.
Unfortunately, though, some teens really struggle during this phase of life – beyond what would (or should) be considered normal adolescent ups and downs. It can be hard, as a parent, to know when to take the attitude of “this, too, shall pass” versus “it’s time to seek professional help for our son / daughter”. Sometimes there’s a significant gray area, and multiple factors need to be considered. But more often than not, the signs are pretty clear – if you’re paying attention; that can be a challenge for parents with harried schedules and plates overflowing with obligations and responsibilities.
Since this phase of your child’s life will have a significant impact on his or her future, the sooner mental health issues are addressed, the better. Following is a list of indicators that your teen likely needs mental health treatment – or at the very least needs an evaluation by a psychologist or other mental health professional. If after reading through them, you’re still hesitant or unsure, at least take your teen in for an evaluation to determine whether or not treatment is necessary.
Remember, many parents tend to view their teens through at least somewhat rose-colored glasses, minimizing or turning a blind eye to serious issues. Sadly, doing so can have very serious repercussions down the road. Better to err on the side of caution than to ignore problems or assume things will work themselves out. If treatment is warranted, it’s absolutely in your teen’s best interest to take that step now rather than later (or even worse, never).
9 Warning Signs Your Teen Needs A Mental Health Evaluation
1 – Your teen is having problems functioning on a day to day basis. One of the primary criterion for practically every disorder listed in the DSM (the diagnostic manual used by mental health professionals) is that the symptoms are severe enough to interfere with day to day functioning or significantly impact at least one or more major area of life (e.g. relationships, school, or work). For example, it’s normal to occasionally feel sad or blue, but it’s not normal to self-mutilate when sad or angry, or become completely withdrawn for weeks at a time.
Signs that your teen isn’t functioning normally may include:
- A notable drop in grades
- Frequent absences or tardiness at school or work
- Decrease in personal hygiene
- Difficulties concentrating
- Bizarre behavior
- Low energy
- Difficulties making decisions
- Inability to cope with minor frustrations
Some psychiatric problems develop quickly, while others develop slowly over time. It’s always important to note any negative changes from your teen’s prior behavior. While it may be temporary, it can also be a sign of something serious.
2 – Your teen appears depressed, sad, withdrawn, or “blue” much of the time, or is often tearful or irritable. Each of these is a potential indicator of depression. As mentioned above, feeling sad or blue from time to time is perfectly normal – it’s part of being human. But it’s important to realize that, even with teens, an often depressed mood is not normal and needs to be addressed.
Many children and teens struggle with undiagnosed depression, suffering in silence for months or even years. Parents and other adults may mistakenly attribute an introverted, quiet demeanor to their personality rather than realizing depression is the real culprit. With proper treatment, a formerly depressed, withdrawn teen can become surprisingly outgoing.
It’s important to note that a significant loss (e.g. the death or loss of a friend, close relative, or beloved pet, or even a major move) can trigger profound feelings of sadness in your teen. However, while grieving is normal, healthy, and necessary, some teens don’t cope well with loss and get stuck in their grief. A major loss can trigger depression as well as exacerbate an existing depression.
While an episode of depression can be short-lived (e.g. a few weeks), it can also last for years – especially if left untreated. It can also lead to other serious problems for teens, increasing their risk for suicide, substance abuse and addiction, and serious academic problems. A drop in grades can make it difficult for them to get into college, and an ongoing or recurring battle with depression can negatively impact their performance if they do get in.
3 – Your teen has intense or rapid mood swings. Adolescent angst – it’s normal, right? Well, yes – to some degree. After all, teens are notorious for being moody, which is often attributed to hormonal changes and fluctuations. However, while occasional or mild moodiness may be normal, frequent intense or rapid shifts in moods shouldn’t be ignored.
Even in teens, a generally upbeat (or at least neutral) mood is a good indicator of healthy psychological functioning and emotional stability. Significant deviations from that may be a sign of psychiatric problems, including depression, bipolar disorder, or borderline personality disorder.
Keep in mind, if your teen is using alcohol or drugs, those substances can also cause erratic or intense mood fluctuations. Significant stress (e.g. parental separation or divorce, or a recent breakup with a boyfriend or girlfriend) can also make your teen moodier than usual. If the mood swings are persistent, an evaluation is warranted. Even if stress is the primary cause (as opposed to a diagnosable disorder), a skilled therapist can help your teen learn healthy coping skills that will be beneficial for years to come. If substance abuse is the cause, early intervention is essential.
4 – Your teen is frequently using alcohol or drugs (which can include prescription drugs, OTC medications, and inhalants) to cope with stress or negative emotions, or fix a problem. It goes without saying that substance use in teens should never be taken lightly. Teens may think it’s expected and acceptable to drink with their friends and experiment with drugs, but the consequences can be devastating. Not only are many substances potentially addictive (leading to more serious long-term problems), they will also impair your teen’s judgment.
With regards to the need for mental health treatment, many teens start drinking or using regularly as a way to “self-medicate” psychiatric symptoms, such as anxiety or depression. They may also turn to illicit substances to enhance athletic performance, quickly drop unwanted pounds, or stay alert while studying for exams. A few beers can quiet racing thoughts, while a friend’s ADHD medication can temporarily boost a negative mood. Your teen may think they’re harmless enough (especially if they are “acceptable” substances, like alcohol or prescription drugs), but it’s an especially serious matter when they’re used to escape, cope, or fix a problem. This is because every time they provide even a little relief or benefit, the desire to use them again is significantly reinforced.
If your teen has a substance abuse problem and a mental health condition, he or she would be a good candidate for what’s known as “dual diagnosis” treatment. Treating only the substance abuse issue or only the mental health disorder will set your teen up for failure. Treating both disorders simultaneously is the best way to ensure a positive outcome and prevent a relapse down the road.
5 – Your teen is preoccupied with his or her weight or physical appearance, and / or has notable issues with eating and food in general. Body image issues and eating disorders often emerge during adolescence. Teens experience significant growth spurts and hormonal changes – both of which can cause problems such as acne and unwanted weight gain (as well as being too thin). They’re also becoming keenly aware of their sexuality. This can be particularly scary for teens with a history of sexual abuse (who may try to thwart the development of curves by starving themselves or binge eat in order to gain enough weight to be undesirable). Other teens feel a desperate need to make themselves more attractive typically involves being thin.
Combine society’s pressure to be thin and beautiful (or muscular and athletic), poor coping skills, and a fragile self-esteem, and you’ve got the perfect recipe for an eating disorder (such as anorexia or bulimia) or another, lesser-known disorder known as “body dysmorphic disorder” (BDD). Eating disorders and BDD not only often go hand in hand; they can also trigger or worsen other disorders, such as depression, anxiety, and substance abuse disorders.
Eating disorders can be especially serious because they often cause significant medical health issues and, for some, permanent physical damage. Anorexia, which is one of the most well-known eating disorders, is also one of the most deadly mental health conditions.
It’s important to note that serious body image issues and a severely dysfunctional relationship with food don’t just affect females. Adolescent males are also vulnerable to developing eating disorders as well as BDD.
6 – Your teen is often anxious or fearful, struggles with obsessions or compulsions, or worries excessively. Anxiety disorders are quite common in children and adolescents. Problems with anxiety can develop gradually or appear suddenly. An abrupt onset is often triggered by a traumatic incident, such as a natural disaster, a school shooting, or being the victim of a violent or sexual assault.
Problems with anxiety often include irrational fears, such as obsessing about having a serious illness or being contaminated by germs, or being terrified by something like spiders or dogs (even if it’s only a photo of a dog or the spider is securely encased in a glass terrarium). Nightmares, nervous habits (e.g. fidgeting, nail biting) and difficulties sleeping are not uncommon in anxious teens.
Occasional fear and worry are normal. However, when anxiety becomes constant, excessive, and / or irrational, it can be paralyzing and interfere with every aspect of your teen’s life.
7 – Your teen is hostile, violent, aggressive, and / or has difficulty managing anger. A teen who’s often angry, irritable, destructive (to self or others), violent, or hostile is a teen who needs help. When any of these behaviors or emotionsoccurs – especially frequently or regularly – it’s a red flag that needs to be taken very seriously.
Angry kids often become angry – and destructive – adults. They’re more vulnerable to accidents, substance disorders, suicide attempts, depression, and abuse or violence towards others. They’re also going to have serious problems at school, at work, and in their relationships.
These particular behaviors and emotions may be due to a variety of factors, including substance use (e.g. steroids, alcohol, or stimulants), trauma, mood disorders, psychosis (e.g. grandiose or paranoid delusions), and personality disorders. Even if your teen doesn’t meet the criteria for a specific disorder, therapy can help him or her learn to manage intense emotions and aggressive impulses.
8 – Your teen has experienced a recent trauma. Although not every teen needs therapy after being subjected to a traumatic event, it’s always wise to have him or her evaluated. Traumatic events are difficult enough for adults with good coping skills and a strong support system. Teens, however, often have yet to fully, or at least sufficiently, develop the skills required to sustain them when their world is turned completely upside down by trauma.
If your teen is having flashbacks, frequent nightmares, experiencing depression or anxiety, having trouble sleeping, or avoiding people, situations, or places that remind him or her of the trauma, treatment is likely necessary.
9 – Your teen is preoccupied with, is threatening, or has attempted suicide. Adolescence is one of the highest risk age groups when it comes to suicide. One of the reasons for this is that teens tend to be very impulsive. They also have a difficult time seeing the bigger picture and realizing that they can and will get through something that – at least in the moment – feels absolutely unbearable, such as the devastating, unexpected end of a romantic relationship.
Suicidal talk, threats, and attempts should always be taken very seriously. Countless parents who have lost a son or daughter to suicide would be quick to say they’d give anything to go back in time and heed the signs – signs that, in retrospect (at least in their minds), should have been so obvious.
Any preoccupation with suicide and death can be a potential clue that your teen is toying with the idea of ending his or her life. Threats are an even stronger indicator. Although some threats are idle, don’t make the mistake of assuming that your teen is just being dramatic. An angry or upset impulsive teen may make a serious attempt, resulting in permanent physical damage or death – even though he or she had no real intention of dying and just wanted to get your attention.
A suicide attempt – even if non-life-threatening – should always be taken very seriously. A naïve teen may think 4 or 5 Tylenol pills or a superficial cut to the wrist are enough to cause death. Don’t underestimate the seriousness of their actions. Additionally, one of the greatest predictors of future suicide attempts is a history of prior attempts.
Keep in mind that suicide isn’t always due to depression. Even when it is, the signs of depression may be subtle. Some teens may get involved in a suicide pact with friends for various reasons. Others may have been depressed, but once they made the decision to end their life they started feeling better. Ironically, a decision to commit suicide can be empowering and actually boost one’s mood, leaving others more baffled than ever when the person – who no longer seemed depressed – ends his or her life.
Any and all suicidal talk, threats, and behaviors warrant an evaluation by a mental health professional as soon as possible.
As a parent, you have a huge responsibility. Teens often lack the insight and maturity to realize when they need help. They also may mistakenly believe that what they’re experiencing is normal or that no one could possibly understand or help them. And, of course, some teens don’t want anyone prying into their personal life. That’s why it’s important to pay attention, keep the doors of communication open, and be ready to take action when needed.
Yes, your child may be mad at you for a while if you make him or her “see some stupid shrink”. But wouldn’t it be far better to endure a brief period of adolescent petulance than watch your precious child suffer for months or years with an undiagnosed, untreated mental health issue – especially one that could have been overcome or significantly alleviated and managed with proper (and early) treatment?
If You Think Your Teen Is Suffering Emotionally Or With A Mental Health Issue, Call Us Now, We Are Here To Help!
Naltrexone is a medication that directly counteracts the intoxicating effects of legal and illegal opioid narcotic substances. Doctors sometimes use the medication to treat people recovering from opioid addiction, but the success of this treatment depends largely on each individual taking his or her naltrexone dose on a regular basis.
In a study published in March/April 2014 in the American Journal on Addictions, a team of Chinese researchers explored the safety of a long-lasting, injectable form of naltrexone that could eliminate some of the concerns about maintaining regular dosing of the medication.
Naltrexone For Opioid Addiction Treatment
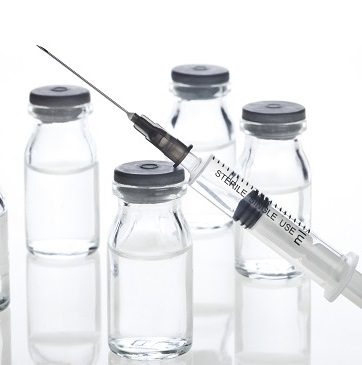 Scientists classify naltrexone with a group of substances known as opioid antagonists. When they enter the bloodstream, all of these substances travel to the sites that normally give opioid drugs and medications access to the brain. Once they reach these sites, opioid antagonists physically block opioids and prevent them from producing their narcotic effects.
Scientists classify naltrexone with a group of substances known as opioid antagonists. When they enter the bloodstream, all of these substances travel to the sites that normally give opioid drugs and medications access to the brain. Once they reach these sites, opioid antagonists physically block opioids and prevent them from producing their narcotic effects.
Naltrexone, in particular, can play a role in opioid addiction treatment because it blocks the effects of opioid substances, lowers the level of opioid craving in recovering addicts and helps diminish the chances that recovering opioid addicts will relapse.
Unlike two opioid-based medications—called methadone and buprenorphine—commonly used in opioid addiction treatment, naltrexone is not a controlled substance. This means that doctors and other qualified health professionals require no special licensing to prescribe it. Many health professionals prescribe an oral form of the medication that patients must take every day.
Injectable Naltrexone
Extended-release, injectable naltrexone is also known as depot naltrexone. Doctors or other qualified professionals administer this medication directly into muscle tissue (typically the gluteus muscles). Instead of dissipating in the bloodstream relatively rapidly like oral naltrexone, extended-release, injectable naltrexone gradually enters the bloodstream for roughly one month and blocks access to the effects of opioid drugs and medications throughout that time.
The main potential benefit of this form of naltrexone is improved compliance with the abstinence goals established in opioid addiction recovery programs. Like the short-acting oral version of the medication, depot naltrexone can trigger severe withdrawal symptoms if given to a recovering addict who still has opioids in his or her system.
For this reason, standard treatment guidelines stipulate that doctors wait at least a week after the verified end of opioid intake to administer the medication. The U.S. Food and Drug Administration approved the sale of an extended-release, injectable naltrexone product called Vivitrol in 2010.
Safety Of Injectable Naltrexone
In the study published in the American Journal on Addictions, researchers from three Chinese institutions used a small-scale trial to assess the safety of injectable depot naltrexone and examine patients’ ability to tolerate the medication.
All told, this trial included 36 people. Twenty-four of these individuals participated in a separate panel. Six people in this panel received a relatively high 400 mg dose of injectable naltrexone, while another six received a relatively low 200 mg dose of the medication. Twelve people in the panel received placebo injections that mimicked either the 400 mg naltrexone dose or the 200 mg naltrexone dose. The remaining 12 study participants were enrolled in a second panel and randomly received either six monthly 400 mg naltrexone injections or placebo injections that mimicked the naltrexone injections.
The researchers found that both the recipients of the 200 mg injections and the 400 mg injections still had medically significant amounts of naltrexone in their bloodstreams one month after dosing. Eleven of the people who received injectable naltrexone had some sort of adverse reaction while using the medication.
The researchers concluded that seven of these reactions were potentially the result of naltrexone exposure; however, they also concluded that none of the observed reactions produced moderate or severe effects.
Overdose Risks?
The authors of the study published in the American Journal on Addictions found that extended-release naltrexone injections deliver steady amounts of the medication for a minimum of one month. They also found that the medication does not accumulate dangerously after multiple monthly injections occur.
Overall, they concluded that extended-release, injectable naltrexone is tolerated well by patients and does not pose any undue safety risks.
On a related note, the federal Substance Abuse and Mental Health Services Administration points out that fatal or non-fatal opioid overdoses sometimes occur in people who receive monthly naltrexone injections but still continue taking opioid substances; however, the same overdose risks also apply to users of oral naltrexone or opioid-based treatment options.
If You Or Someone You Love Is Struggling With Addiction, Call Us Now! Help Is Waiting.
See Why Naltrexone Helps Reduce Amphetamine Use Could This Be An Effective Treatment For Your Addiction?
According to the Centers for Disease Control and Prevention, tobacco use is the leading preventable cause of death in the United States. This is why helping people quit smoking is such a priority. Unfortunately, most smokers find it very hard to give up the habit. The Smoking Treatment for Ontario Patients (STOP) program—funded by the Ontario Ministry of Health and Long-Term Care—is one approach that manages to increase quit-rates by providing nicotine patches and psychological treatment to smokers, and could serve as an example for U.S.-based organizations. The initiative started in 2005 and now runs numerous times per year, offering smokers the opportunity to break free of their addictions and get healthy.
Why Is It So Hard To Quit Smoking?
 Although tobacco is a widespread and legal substance, quitting it is hard for many of the same reasons that it’s difficult to stop using illegal drugs. Nicotine—the addictive component of cigarettes—releases dopamine in the brain, the neurochemical responsible for the majority of addictions. When the body gets accustomed to it, the external “boost” that smoking provides stops, and this leads to an imbalance in brain chemicals followed by unpleasant symptoms. The problem is compounded by the fact that research indicates “cold turkey” (unsupported) quitting is the most popular method, but is a considerably less successful strategy than counseling, medications and nicotine replacement therapy (like gums or patches). In short, smokers—with an already difficult task ahead of them—often try to quit by themselves, which is statistically the least successful method.
Although tobacco is a widespread and legal substance, quitting it is hard for many of the same reasons that it’s difficult to stop using illegal drugs. Nicotine—the addictive component of cigarettes—releases dopamine in the brain, the neurochemical responsible for the majority of addictions. When the body gets accustomed to it, the external “boost” that smoking provides stops, and this leads to an imbalance in brain chemicals followed by unpleasant symptoms. The problem is compounded by the fact that research indicates “cold turkey” (unsupported) quitting is the most popular method, but is a considerably less successful strategy than counseling, medications and nicotine replacement therapy (like gums or patches). In short, smokers—with an already difficult task ahead of them—often try to quit by themselves, which is statistically the least successful method.
Physical Withdrawal Symptoms Of Nicotine Withdrawal
Like with other drugs, when you stop consuming nicotine you may feel a wide range of physical symptoms. The most common smoking withdrawal symptoms are agitation, irritability, weight gain, depression and anxiety. The negative symptoms come on because the individual is no longer getting the nicotine he’s become dependent on, and the brain knows it, creating cravings in an attempt to make the individual succumb to temptation and give it another hit of nicotine.
Psychological Challenges Of Quitting Smoking
Although the physical withdrawal symptoms add to the discomfort of quitting smoking, the psychological effects are what drive many ex-smokers to relapse. Smoking, like other drug addictions, is a poor coping strategy for dealing with everyday problems, and when these problems return, the individual is at particular risk for relapse. Both internal and external “triggers” to smoke can make the process more difficult, with internal factors including things like stress and depression and external ones including things like being around a friend who smokes or taking a work break that you previously used for smoking. These things push the individual back to smoking, and in combination with the physical withdrawal symptoms, they make the process of quitting extremely challenging.
Benefits Of Initiatives Like STOP
These issues are what make initiatives like STOP so worthwhile. The core selling point of STOP is that attendees receive five weeks’ worth of free nicotine patches, which ordinarily cost around $30 per week, meaning they save around $150. This removes what some see as a financial barrier to getting the support they need, but the support also takes the psychological elements into account. Each qualifying smoker is also eligible to attend workshops and receive ongoing support to help manage triggers and cravings.
This broad range of support contributes to the impressive success rates enjoyed by the initiative. Oxford County’s tobacco control coordinator Dominique Bruce points out that those in the program have a quit rate that’s 50 percent higher than those not in the program. She also points to the cost savings and psychological support offered by the program. “If you slip up, you need to remember it’s just a slip up, not a fail,” Bruce said.
The Right Way To Help People Quit Smoking
There are many lessons that can be learned from programs like STOP, and although this initiative is in Canada, U.S.-based stop smoking initiatives can take a cue from the approach and work to reduce the preventable diseases and deaths caused by smoking. The smokers themselves face the biggest challenges, but with the right support and the guidance to help them push through the difficult periods, they have the ability to kick their tobacco addiction for good. As long as we understand the challenges inherent in quitting smoking—or kicking any addiction—we can find the compassion to help those in need and the wisdom to do so in the most effective way possible.
Addiction specialists and other health professionals have a range of medication-based options for helping people affected by alcoholism. However, even when they receive one of these medications, some recovering alcoholics still lapse back into heavy alcohol consumption. In a study published in April 2014 in the journal Alcoholism: Clinical & Experimental Research, researchers from three German institutions assessed the effectiveness of individualized psychotherapy in recovering alcoholics who don’t respond sufficiently to medication-based treatment. Specifically, the researchers examined the usefulness of a form of individualized therapy called cognitive behavioral therapy.
What Medications Can Help Alcoholics?
 As of 2014, the U.S. Food and Drug Administration has approved a trio of medications for use in people recovering from alcoholism: naltrexone (Vivitrol), disulfiram (Antabuse) and acamprosate (Campral). Naltrexone is an anti-opioid medication that also blocks the chemical reactions responsible for triggering pleasurable sensations and alcohol cravings in drinkers. Disulfiram deters alcohol consumption by exaggerating the unpleasant chemical reactions associated with the breakdown of alcohol inside the body. Acamprosate makes chemical changes inside the brain that typically lessen the intensity of the alcohol withdrawal symptoms that commonly contribute to relapse risks in recovering alcoholics. Doctors also sometimes use a fourth medication, called topiramate (Topamax), not initially intended for use in alcoholism treatment. This anti-seizure compound also makes changes in the brain’s chemical environment that can help lower the odds that recovering alcoholics will take a drink.
As of 2014, the U.S. Food and Drug Administration has approved a trio of medications for use in people recovering from alcoholism: naltrexone (Vivitrol), disulfiram (Antabuse) and acamprosate (Campral). Naltrexone is an anti-opioid medication that also blocks the chemical reactions responsible for triggering pleasurable sensations and alcohol cravings in drinkers. Disulfiram deters alcohol consumption by exaggerating the unpleasant chemical reactions associated with the breakdown of alcohol inside the body. Acamprosate makes chemical changes inside the brain that typically lessen the intensity of the alcohol withdrawal symptoms that commonly contribute to relapse risks in recovering alcoholics. Doctors also sometimes use a fourth medication, called topiramate (Topamax), not initially intended for use in alcoholism treatment. This anti-seizure compound also makes changes in the brain’s chemical environment that can help lower the odds that recovering alcoholics will take a drink.
Cognitive Behavioral Therapy
Practitioners of cognitive behavioral therapy (CBT) help their patients/clients identify the underlying feelings, perceptions and actions that contribute to dysfunctional behavior in stressful situations. After making this identification, the individual can gradually learn a new set of feelings, perceptions and actions that don’t help trigger destructive behaviors. In the context of addiction treatment, CBT practitioners specifically help their patients/clients learn to do such things as anticipate the situations likely to increase the urge to use drugs or alcohol, learn how to cope with those situations without using drugs or alcohol, identify substance-using urges as soon as possible and accurately weigh the pros and cons of using drugs or alcohol.
Cognitive behavioral therapy is suitable for use in both individualized and group formats. In addition, the therapy can be used on its own or in combination with medication-based addiction treatment. In addition to alcoholism, forms of addiction addressed by CBT include addiction to the stimulants methamphetamine and cocaine, marijuana addiction and addiction to the nicotine contained in cigarettes and other tobacco products.
Usefulness In People Not Helped By Medication
In the study published in Alcoholism: Clinical & Experimental Research, researchers from Germany’s Freiberg University, Tubingen University and Heidelberg University used an examination of 109 individuals to assess the effectiveness of an individualized cognitive behavioral approach in helping recovering alcoholics who don’t receive enough benefit from medication-based treatment. All of these individuals were alcohol program participants who had experienced severe relapses back into drinking after taking an alcoholism medication, or after receiving a placebo that mimicked the appearance of an alcoholism medication. During the study, half of the participants continued to receive a standard combination of medication and medical symptom management. The other half received a combination of medication, medical symptom management and cognitive behavioral therapy conducted on an individualized basis.
The researchers analyzed the effectiveness of individualized CBT in all of the participants originally assigned to the therapy group, as well as the effectiveness of the approach in all of the participants who actively engaged in therapy. After completing these analyses, they concluded that the recovering alcoholics who actively engaged in the CBT process received a substantial benefit from the therapy and experienced improved treatment outcomes when compared to the recovering alcoholics who received only medication and medical symptom management.
The chief measurement used to compare the effectiveness of the combination of medication and individualized cognitive behavioral therapy to the effectiveness of medication without CBT was the number of days recovering alcoholics could successfully avoid experiencing another severe relapse. The authors of the study published in Alcoholism: Clinical & Experimental Research concluded that those program participants who actively embrace the goals of individualized CBT can potentially increase the number of days between relapses if they combine the therapy with an alcoholism medication. In line with this conclusion, they believe that alcohol programs may see significant improvements in their patients’/clients’ relapse-related outcomes if they offer access to non-medication-based therapy early in the treatment process.
Read How Do Recovering Alcoholics Respond To Baclofen?
26 May 2014
Marijuana Habits May Dictate Dependence
If scientists can develop an understanding of how a casual user sometimes becomes an addict while others do not, they may be more equipped to prevent addiction. Understanding how casual marijuana experimentation turns into addiction may help in prevention and intervention strategies, in addition to shaping public policy. A recent study identified behavior patterns that may determine whether a person develops an addiction to marijuana.
 The study, which was led by Peggy van der Pol of the Trimbos Institute of the Netherlands Institute of Mental Health and Addiction, suggests that theories about whether increased levels of the psychoactive ingredient delta-9-tetrahydrocannabinol (THC) can influence addiction may not be relevant. With varying potencies of THC available in marijuana, the researchers wanted to see whether potency, habits of the user or both determined the likelihood of them becoming addicted.
The study, which was led by Peggy van der Pol of the Trimbos Institute of the Netherlands Institute of Mental Health and Addiction, suggests that theories about whether increased levels of the psychoactive ingredient delta-9-tetrahydrocannabinol (THC) can influence addiction may not be relevant. With varying potencies of THC available in marijuana, the researchers wanted to see whether potency, habits of the user or both determined the likelihood of them becoming addicted.
Some scientists have argued that even when THC is more potent users may compensate by inhaling less. However, the authors say there is a much more relevant predictor.
While smokers of more potent pot receive more THC now than users of older generations of marijuana, the style of smoking is a better predictor of which users are likely to become dependent. Van der Pol explains that while every drug carries risk, the more potent forms of marijuana cause the user to take in more THC.
How Is Dependence Developed?
Other studies have focused on frequency of use when examining how dependence developed, as well as THC levels. Van der Pol’s team looked at data from 98 young adults enrolled in a long-term study on regular marijuana use in the Netherlands. The users were recruited from cannabis dispensing coffee shops, as well as through referrals. The participants all reported using marijuana at least three days per week in the previous year. One in three of the participants met criteria for dependence at baseline. The participants were mostly men and were an average age of 23.
Eighteen months after recruitment, and at another follow-up point at three years, the participants were interviewed about their cannabis use, and were even asked to smoke during the interview.
The researchers documented the specific behaviors each participant demonstrated, from rolling their joints to how often they puffed on the joint. To provide a picture of regular behaviors, the participants were asked to bring their own cannabis and roll their own joints.
The smokers who used more potent pot containing higher concentrations of THC did not roll weaker joints. Instead, they used more pot in each joint when compared to users of less-potent marijuana.
The potent pot users did inhale less smoke and had a slower pace of smoking when compared with their peers. However, these adjustments weren’t sufficient to compensate for the higher level of THC in the marijuana.
Instead of THC exposure, the study results showed that only behaviors specific to smoking were predictors of dependence. How many puffs a smoker took, and the amount they smoked, were the only strong predictors of dependence at three years following the initial examination.
The study’s findings may have an immediate impact on how users are educated about marijuana dependence. New users may be exposed to a stronger potency of marijuana and consume high levels of THC.
Find Out If Marijuana Legalization Is Leading To Increased Use
Twelve-step programs are mutual self-help programs that use a combination of gradual goals (i.e., steps) and peer support to help recovering substance addicts establish and maintain a long-term commitment to avoiding further substance use. However, not all people who join these programs attend regularly or successfully abstain from substance intake. In a study published in May 2014 in the journal Addiction, researchers from the U.S. and Norway assessed the effectiveness of a technique called motivational intervention in helping 12-step participants increase their program involvement and their ability avoid substance relapses.
12-Step Approach
 The 12-step approach was initiated in the 1930s with the formation of Alcoholics Anonymous. Participants in 12-step-based programs commit to a progressive series of actions designed to help them recover from active involvement in the use of alcohol or other substances of abuse. These actions including admitting a lack of self-control over addictive behaviors, making a call to a higher or greater power to assist in the recovery process, examining and atoning for damaging conduct while under the influence of drugs or alcohol, and eventually providing assistance to others not as far along the path of recovery. As a rule, 12-step programs rely heavily on peer sponsorship provided by longer-term members. The 12-step approach is widely used and has proven effective as an aid to the substance recovery efforts carried out in treatment centers that deal with problems such as alcohol addiction, cocaine addiction and opioid narcotic addiction.
The 12-step approach was initiated in the 1930s with the formation of Alcoholics Anonymous. Participants in 12-step-based programs commit to a progressive series of actions designed to help them recover from active involvement in the use of alcohol or other substances of abuse. These actions including admitting a lack of self-control over addictive behaviors, making a call to a higher or greater power to assist in the recovery process, examining and atoning for damaging conduct while under the influence of drugs or alcohol, and eventually providing assistance to others not as far along the path of recovery. As a rule, 12-step programs rely heavily on peer sponsorship provided by longer-term members. The 12-step approach is widely used and has proven effective as an aid to the substance recovery efforts carried out in treatment centers that deal with problems such as alcohol addiction, cocaine addiction and opioid narcotic addiction.
Motivational Interventions
Many people who enter substance recovery programs do so with mixed feelings about the recovery process. In fact, significant numbers of program participants enter treatment only at the urging of others. People with ambivalent or hostile feelings toward substance recovery commonly fail to participate fully in their programs, meet the specific objectives that programs set for their clients/patients or successfully complete their program involvement. Motivational interventions are designed to help program participants uncover the mixed or negative feelings they may have about substance recovery, and also to help them change their minds and become more willing and proactive in their treatment. As a rule, practitioners of motivational interventions work cooperatively with clients/patients in an interactive process that strives to avoid a confrontational or antagonistic atmosphere. While a motivational intervention can help at almost any stage of treatment, it typically has its biggest impact in the initial stages of recovery.
Usefulness In 12-Step Programs
In the study published in Addiction, researchers from Stanford University, the Department of Veterans Affairs and Norway’s University of Oslo and Sorlandet Hospital used an examination of 140 Norwegians receiving treatment for alcoholism to assess the usefulness of motivational interventions in promoting involvement in 12-step programs. All of these study participants were in inpatient facilities for alcohol detoxification. Half of the participants received a motivational intervention called 12-step facilitation in two 30-minute sessions. This form of intervention is designed to increase clients’/patients’ level of comfort with 12-step involvement. The facilitation sessions provided during the study included detailed explanations of how substance addicts lose control over their behaviors, a DVD on the 12-step process created by Alcoholics Anonymous and immediately available resources for making direct contact with 12-step groups. The other half of the study participants received only basic advice on 12-step resources in a brief informational session.
Six months after the study participants concluded their involvement in inpatient detoxification, the researchers compared the level of 12-step involvement among the people who received motivational interventions to the level of involvement among the people who only received brief advice on 12-step resources. They concluded that the participants who received motivational interventions were significantly more likely to attend 12-step meetings than those who received only brief advice. They also concluded that the motivational intervention group used both alcohol and drugs on fewer total days than the brief advice group.
Despite the increased 12-step involvement and fewer days of substance use, the authors of the study published in Addiction concluded that the recovering alcoholics who received motivational interventions did not remain abstinent from substance use any more often than their counterparts who received brief advice on available 12-step resources. In addition, motivational intervention did not lead to a decrease in the severity of alcohol-related symptoms. Still, the authors note that, since motivational intervention recipients do attend 12-step meetings more often and use drugs and alcohol on fewer days, the technique may prove useful as part of the recovery process for alcoholics who go through alcohol detoxification.
American attitudes toward drugs and drug users are changing. A few decades ago Americans wanted stiff mandatory sentencing for drug users and dealers. This has led to crowded prisons, strained state budgets and little headway in terms of changing drug behavior. A recent poll revealed that two-thirds of Americans are in favor of drug treatment rather than criminal prosecution.
Jail Or Rehab?
 The Pew Research Center has polled the country on this subject and says that Americans would rather see offenders with no history of violence get help as opposed to jail time. Pew talked to 1,821 U.S. adults, finding that 67 percent felt the emphasis should shift toward treatment, just over 26 percent advocated for a continued focus on punishment and seven percent said they could not decide on which course was best. The poll was conducted for one week in February 2014.
The Pew Research Center has polled the country on this subject and says that Americans would rather see offenders with no history of violence get help as opposed to jail time. Pew talked to 1,821 U.S. adults, finding that 67 percent felt the emphasis should shift toward treatment, just over 26 percent advocated for a continued focus on punishment and seven percent said they could not decide on which course was best. The poll was conducted for one week in February 2014.
The two-thirds majority felt mandatory sentencing should not be applied to small scale crime, especially if it was marijuana-related. This is a significant shift in public opinion since as recently as 2001 more than half of polled Americans still supported strong penalties and prison sentencing for drug offenses, including marijuana.
The President and his administration have been lending voice to the move away from harsh mandatory sentencing. Prosecutors show less support for the idea, but so far President Obama has enjoyed Congressional support from both sides of the aisle when he suggests eliminating most mandatory sentences.
Marijuana Legalization
The poll discovered that 49 percent support the legalization of medical marijuana use, and 39 percent support legalizing recreational use. Just 16 percent maintain that marijuana should continue as an illegal substance in this country. But nearly all those polled, on both sides of the issue, expressed the belief that marijuana will eventually become a legal substance in America.
This is a notable change in public sentiment. Back in 2010 Pew reported that 41 percent supported legalization, while a majority – 52 percent – still thought the drug should be illegal. The new poll is essentially a flip of prior attitudes. At the moment medical marijuana use is legal in 20 states and recreational use is legal in two.
The prevailing attitude among Americans seems to be that a person should be free to use marijuana as long as they do it in the privacy of their own home. Even though they favor loosening the laws surrounding marijuana use, Pew reported that 63 percent did not want people to use it in public, and 44 percent did not want to have a dealer present on the street where they live.
Americans appear ready to give up on the fight against marijuana, but they still have some misgivings. Many are concerned that when marijuana is more available more young people will be likely to give it a try. And even though the country is moving away from sending drug sellers and users to prison, they still think drugs are an issue. Over 50 percent of those polled said they thought drug abuse was a “serious problem,” and just over 30 percent said drug abuse is a “crisis.”
From the White House to ordinary households, the feeling in America seems to be “let’s put small scale drug users into treatment, rather than prison.” On the one hand Americans are ready to allow fellow citizens free access to marijuana, but at the same time they worry about where that policy may lead. The majority of Americans seem to feel that fear of punishment has not been effective in reducing drug abuse and are ready to try a new approach.
Two trends in substance use are affecting the bottom line among small businesses. One is a significant increase in the abuse of prescription painkillers. The other is the increased use of marijuana as a result of increased deregulation.
According to a survey conducted by Employers Holdings Inc., one out of 10 small businesses report having employees show up to work while under the influence of at least one controlled substance, with lost productivity and potential insurance costs affecting the bottom line of the business.
Many companies require that employees provide a clean urine or blood sample both at hiring and at the discretion of the employer for random testing. However, in some cases, the employee may arrive at work visibly affected by a substance.
Prescription Drug Use
 Opioid misuse has been on the rise. The U.S. Centers for Disease Control and Prevention report that more overdose deaths are now recorded for prescription opioids than for heroin or cocaine.
Opioid misuse has been on the rise. The U.S. Centers for Disease Control and Prevention report that more overdose deaths are now recorded for prescription opioids than for heroin or cocaine.
Prescription drug abuse often begins with a legitimate pain problem, often resulting from a serious injury or chronic disease. The patient may not receive adequate warnings, or they may not exercise the necessary caution in avoiding addiction to the drug.
In other cases unlocked medicine cabinets provide an opportunity for forgotten pills to be pilfered. Opioids can produce the same high as heroin, and they are a popular choice for experimentation. Many users mistakenly believe that because the drugs are obtained through a prescription from a doctor they aren’t as dangerous as street drugs.
Instead, experts say, the use of opioids can be just as dangerous as street drugs. Common reactions include a racing pulse or stroke. In some cases users may combine the drugs with other pills to make a unique cocktail and significantly increase the likelihood that they will experience negative side effects.
One potential danger of using opioids is that when a user runs out of opportunities to obtain prescription opioids from the medicine cabinets of friends and relatives the addiction may be fully developed. Buying pills on the street can be very expensive, costing $80 to $100 per pill. The remedy, in too many cases, is to start using heroin. Heroin is available and cheap, compared to prescription painkillers.
Marijuana Use Increasing
The increasing legalization of marijuana is also becoming a challenge for employers. Many don’t believe that their employees are able to work safely while under the influence, and are struggling to adequately prevent the substance from impacting their business, the safety of their employees and those they interact with on any given day.
With states beginning to allow the possession and use of marijuana, the impact is being felt by small businesses. In Colorado, where marijuana sales are booming, employers are scrambling to compensate for the impact the drug can have on their employees and their businesses.
More than half of employers surveyed even mentioned over-the-counter medications as a particular danger to employees and those around them. Three-quarters of the employers agreed that marijuana, prescription painkillers, alcohol and illicit narcotics presented a danger to their employees.
The survey was conducted by International Communications Research, who interviewed 502 small businesses that were nationally representative of small businesses that have fewer than 100 employees.
Find Out If Some Businesses Reward Drug Abuse


